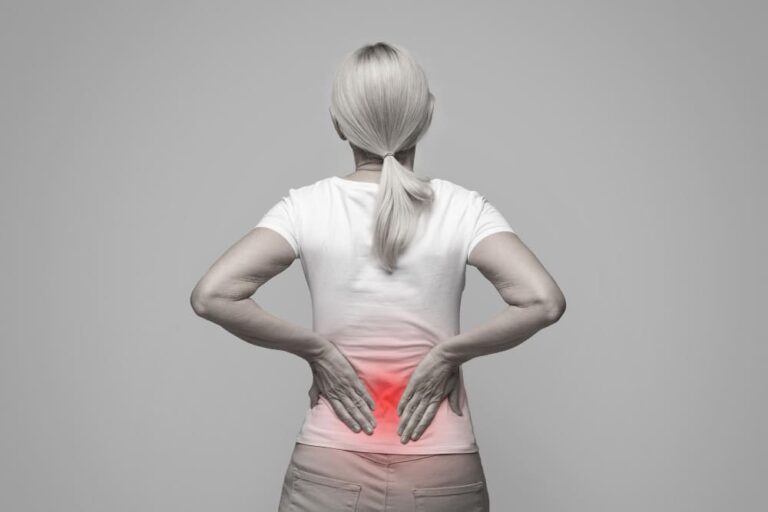
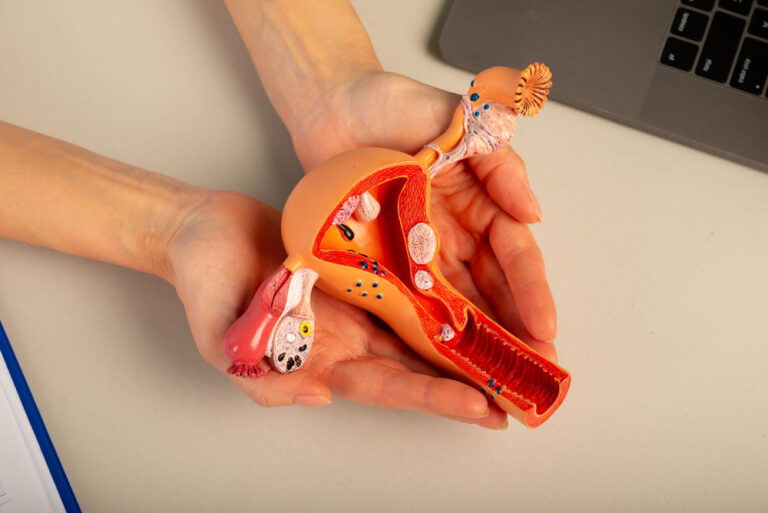
You’re tired of unexplained lower back pain, heavy menstrual bleeding, and constant pelvic discomfort. The worry grows every month as the pain gets worse and starts to affect your work, sleep, and relationship. To finally get answers to the question does adenomyosis cause back pain? you first need to understand what is happening inside your uterus and which treatments actually bring long‑term relief.

Table of Contents
Does adenomyosis cause back pain? Lower back pain and referred pain explained
Adenomyosis is a common gynecological condition where the endometrial lining that should stay inside the cavity of the uterus starts to grow into the muscular wall of the womb. This abnormal endometrial tissue still responds to hormones during the menstrual cycle, so it thickens, breaks down, and bleeds, but it is trapped inside the muscle.
This process creates inflammation, swelling, and pressure in the uterus. For many women, this adenomyosis pain is not limited to the pelvis. Because pelvic nerves and lower back nerves are closely linked, the brain can misread the source of the pain. This is called referred pain and it is one of the key reasons why adenomyosis can cause persistent lower back pain.
Patients often report:
- Deep, aching pain across the lower back during or before menstruation
- Cramps that start in the pelvis and spread to the back and upper thighs
- Pain that gets worse over time and becomes almost chronic, not only during periods
So, yes—adenomyosis can cause back pain, especially around the time of menstruation, and this pain may be mistaken for a spine or muscle problem if the underlying uterine condition is not recognized.
What is adenomyosis? A common uterine condition in women
To understand why adenomyosis hurts so much, it helps to look at the structure of the uterus. The womb has:
- An inner lining called the endometrium
- A thick muscle wall called the myometrium
In adenomyosis, endometrial tissue grows inside that muscle wall. This inflammatory condition can enlarge the size of the uterus, sometimes making it feel bulky or tender on examination. Some women describe feeling as if they are “carrying a heavy stone” in the pelvis.
Typical signs and symptoms of adenomyosis include:
- Very painful menstrual periods (dysmenorrhea)
- Heavy or prolonged menstruation, sometimes with blood clots
- Constant pelvic cramps and pressure
- Pain during intercourse (dyspareunia)
- Pelvic discomfort that radiates to the back or legs
Because the symptoms overlap with other uterine conditions like fibroids, endometriosis, and pelvic inflammatory disease, adenomyosis is often under‑diagnosed. Yet it is a common condition in women in their 30s, 40s, and perimenopause, especially those who had previous pregnancies or uterine surgeries.
How adenomyosis pain develops: from pelvic discomfort to lower back pain
Adenomyosis pain is not “in your head.” It has a clear physical cause inside the body.
During the menstrual cycle, the misplaced endometrial tissue inside the muscle bleeds and swells. This triggers:
- Inflammation and release of pain chemicals
- Strong uterine muscle cramps as the uterus tries to expel blood
- Increased pressure in the pelvis, especially when the uterus is enlarged
These changes can irritate surrounding nerves and ligaments. The pelvis, lower abdomen, and lower back share nerve pathways, so your brain may interpret deep pelvic pain as pain in the lower back muscles or even in the buttocks.
Many patients report that:
- Back pain is worst just before and during menstruation
- Pain improves a bit after periods, then returns the next cycle
- Over time, the discomfort becomes more constant and affects daily life
Because of this pattern, some women spend years treating only their back with physiotherapy, painkillers, or muscle relaxants, while the true gynecological disease in the uterus remains untreated.
Adenomyosis vs other uterine conditions and causes of similar symptoms
Adenomyosis is often confused with endometriosis and uterine fibroids because they share many symptoms, such as pelvic cramps, heavy bleeding, and pain during intercourse. However, they are different uterine conditions:
- Adenomyosis: Endometrial tissue grows within the uterine muscle wall.
- Endometriosis: Endometrial‑like tissue grows outside the uterus on organs such as the ovaries, bowel, or pelvic wall.
- Fibroids: Benign tumors made of smooth muscle that grow in or on the uterus.
All three may cause lower back pain, which is why it is important to look at the causes of similar symptoms before choosing a treatment.
For example:
- Adenomyosis often causes a diffusely enlarged uterus and heavy, painful periods.
- Fibroids may cause pressure symptoms (like frequent urination) if they reach a large size.
- Endometriosis can lead to severe pain, especially during menstruation, and sometimes fertility problems.
Sometimes, women even have adenomyosis and fibroids together, which makes the picture more complex. A careful diagnosis by a specialist in women’s health and interventional radiology helps distinguish these conditions and choose the best therapy.
When heavy menstrual bleeding and cramps signal a symptom of adenomyosis
Not every heavy period means adenomyosis, but certain patterns should not be ignored. Typical symptoms of adenomyosis that should prompt you to seek medical advice include:
- Heavy menstrual bleeding that soaks pads or tampons quickly
- Menstrual periods that last more than 7 days or feel prolonged
- Passing large blood clots during menstruation
- Severe cramps that interfere with daily activities or work
- Feeling exhausted, weak, or dizzy because of blood loss (possible anemia)
These symptoms are not just an inconvenience; they affect your quality of life, mood, sleep, and relationships. Many patients report avoiding social events, intimacy, or travel because of fear of bleeding or pain.
Over time, chronic inflammation and repeated blood loss can impact overall health, making you more tired and less able to exercise or care for your family. Recognizing these warning signs early helps you seek treatment before the condition becomes harder to control.
How adenomyosis is diagnosed and why accurate diagnosis matters
There is no single blood test that confirms adenomyosis. Instead, doctors use:
- Medical history: Your pattern of pain, bleeding, and other symptoms
- Physical examination: Feeling an enlarged, tender uterus
- Ultrasound: To check the uterine wall, fibroids, and other pelvic structures
- MRI: Often the best imaging tool to show adenomyosis clearly
Many patients report years of being told their pain is “normal period pain” before getting a proper diagnosis. If your symptoms are severe or getting worse, you have the right to ask for further evaluation, especially if you suspect a gynaecological condition such as adenomyosis or endometriosis.
Accurate diagnosis is essential because the right treatment can relieve symptoms without removing the uterus. Today, interventional radiology offers organ‑preserving options that were not widely available a generation ago.
Non‑surgical treatment: uterine artery embolization for adenomyosis pain
In the past, many women with severe adenomyosis were offered only hysterectomy (surgical removal of the uterus). While surgery may still be necessary in some cases, it is not the only option.
Uterine artery embolization (UAE) is a non‑surgical, image‑guided treatment performed by an interventional radiology consultant such as Dr. Samir Abdel Ghaffar. It is used to treat both adenomyosis and uterine fibroids.
How it works, in simple terms:
- A tiny tube (catheter) is guided through an artery in the wrist or groin.
- Using live imaging, the doctor navigates to the uterine arteries that supply blood to the diseased tissue.
- Very small particles are injected to block the blood flow to the adenomyosis and fibroids.
- Over time, the treated tissue shrinks, inflammation reduces, and the adenomyosis pain and heavy bleeding often improve.
Benefits of uterine artery embolization include:
- No large surgical cuts, so less muscle damage and faster recovery
- The uterus is preserved, which matters to many women
- Most patients go home the same day or the next day
- Many report clear relief from pelvic cramps, lower back pain, and heavy periods
Interventional radiology also treats many other conditions in the body, such as liver tumors and prostate enlargement, using similar minimally invasive principles.
Frequently Asked Questions
What does an adenomyosis flare up feel like?
Flares mimic intense period pain: sharp pelvic cramps, heavy bleeding, lower back throbs, nausea, and fatigue. It peaks mid-cycle, lasting days, with bloating and leg aches from pressure.
What are the four stages of adenomyosis?
Staging is diffuse or focal: 1) Early superficial invasion; 2) Moderate myometrial involvement; 3) Deep junctional zone growth; 4) Extensive uterine enlargement with cysts. MRI grades severity.
Can uterus problems cause lower back pain?
Yes, conditions like adenomyosis, fibroids, or endometriosis irritate nerves, referring pain to the lower back. Uterine enlargement presses on ligaments, worsening with activity or full bladder.
Where does it hurt when you have adenomyosis?
Pain centers in the lower abdomen and pelvis, radiating to the lower back, thighs, and rectum. It’s diffuse, cycle-tied, and sharp during flares or sex.
Ready for relief? Contact Dr. Samir Abdel Ghaffar, expert in non-surgical uterine artery embolization for adenomyosis and fibroids.
London, UK:
Clinic: +44 20 8144 2266
WhatsApp: 00447377790644
Egypt (Cairo):
Booking/WhatsApp: 00201000881336
Take the first step toward less pain and better days.